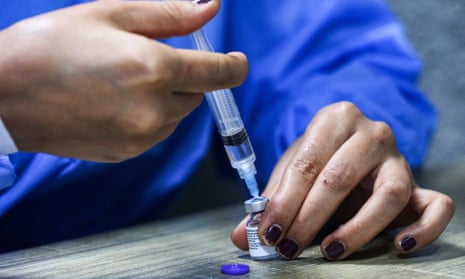
A single dose of either the Oxford/AstraZeneca or the Pfizer/BioNTech vaccine generates a big protective antibody response against the coronavirus in people 80 and over, researchers have found.
The first study to look at the comparative performance of the two vaccines that have been in use in the UK in recent months shows that 93% of people develop antibodies against the coronavirus spike protein by five to six weeks after a single Pfizer jab, and 87% after a single AstraZeneca one.
But the researchers from the UK Coronavirus Immunology Consortium, which includes scientists from 20 different centres, found a difference when it came to the cellular response elicited by the vaccines. That is the generation of T-cells that help fight the virus.
The AstraZeneca vaccine had a greater effect – with 31% of people developing T-cells against the spike protein compared with 12% of those who had the Pfizer jab. People who had the AstraZeneca shot also had a stronger cellular response.
The findings suggest that the UK’s policy of a 12-week wait between doses is safe, as the most vulnerable age group does develop a strong antibody response to the vaccines well before the second delayed dose. They say more work is needed to find out whether the difference in cellular response is significant.
“It is important to understand how the immune response generated by Covid-19 vaccines varies with age, the delay between doses, and the type of vaccine administered,” said Paul Moss, professor of haematology at the University of Birmingham and the consortium’s principal investigator.
“As far as we know, this study is the first of its kind to compare both antibody and T-cell responses following a single dose of either the Pfizer or AstraZeneca vaccine in any age group. The findings are reassuring because many countries, including the UK, have chosen to delay administering second doses.”
The study, published online as a preprint by The Lancet, has not yet been peer-reviewed. The researchers analysed blood samples from 76 people, age 80 to 99, who had a single dose of the Pfizer jab, and 89 who had the AstraZeneca vaccine.
Dr Helen Parry, academic clinical lecturer at the University of Birmingham and the first author of the paper, said it is important to study what is happening to the immune systems of older people after vaccination.
“The Covid vaccine response in older people is of particular interest to us because we know that the function of the immune system deteriorates with age. You don’t always respond as effectively to vaccines as the younger population, but also older individuals do have the highest risk for severe Covid,” she said.
“The UK and some other countries have opted to delay the second dose, in order to accelerate population coverage. So in this high-risk group for Covid-19, we think it’s really important that we study immune responses to the different vaccine platforms, but also the different schedules that are going forward.”
Eight people who had already had Covid-19 had a very strong immune response after a dose of vaccine – a nearly 700-fold increase in antibodies and four-fold in T-cells. “Previous natural infection really enhances the immune responses to the vaccine but all patients should still receive the two vaccines,” said Parry.
Antibody responses are important against infection and reinfection, said Moss, “but the cellular response is more subtle”. T-cells might protect against severity of disease, but they may also be less susceptible than antibodies to loss of immunity from variants.
“I think people are confident that variants will only lose 10% to 20% of the cellular response, whereas they can lose a lot more of the antibody response. It’s about how the immune system works,” he said.
One possibility for the future is that vaccines could be “mixed and matched”, so that people could have one jab that elicits a stronger cellular response and one that produces a higher antibody count. A trial looking at combining these two vaccines in this way has just been extended to include the Moderna and Novavax jabs as well.
Meanwhile a new study by the NHS and the University of Manchester found that older people who had received the Pfizer jab were less likely to be admitted to hospital. Researchers examined data on more than 170,000 people aged 80 to 83 who received the vaccine between 15 and 20 December last year, at the time it was the only jab in use in the UK. They found that between 35 and 41 days after the first vaccine, emergency admissions were 75% lower in the vaccinated group when compared with unvaccinated 76 to 79-year-olds.