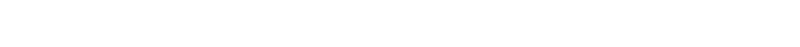Mallory Goepel wipes away tears as she and her husband, Kyle Goepel, introduce baby Demi to her siblings Will Goepel, 2, and Gia Goepel, 4, at their home in Des Peres on Thursday, July 16, 2020. Goepel gave birth to Demi via C-section on June 26, 2020, when she was on a ventilator being treated for COVID-19. Demi was discharged on Thursday from the intensive care unit at St. Louis Children’s Hospital and allowed to go home to meet her siblings for the first time. Photo by David Carson, dcarson@post-dispatch.com
DES PERES — Mallory Goepel expects that one day, it’s going to hit her. And when it does, she’ll likely collapse into a puddle on the floor.
For now, though, Goepel feels nothing but gratitude — “grateful that I’m alive, grateful that my daughter is OK, grateful that my husband and my kids are OK, grateful to be home.”
Goepel, 35, of Des Peres, brought her newborn home from intensive care on Thursday, three weeks after Goepel was placed on a ventilator because of COVID-19. Demi Penelope, delivered early by cesarean section, wasn’t supposed to be born until Aug. 12.
Before going into surgery and getting the ventilator, Goepel had to say her “just-in-case” goodbyes to her husband and two children, ages 2 and 4, through a video chat. Knowing the odds of waking up after requiring a ventilator were not good, Goepel was petrified she’d never see her family again.
People are also reading…
And while she went through her ordeal, she didn’t see them: Her husband and children tested positive for coronavirus, as well.
But Goepel had another family with her. She works as a nurse practitioner in the neonatal intensive care unit at St. Louis Children’s Hospital. As she was wheeled to the operating room, she was comforted by her close team of co-workers waiting to take Demi to the NICU.
Christine Kilian, the nurse manager, remembers the frightened look on Goepel’s face.
“I gave her a thumbs-up and said, ‘You are going to be great’ and ‘I’ll be praying for you the whole time,’” Kilian said. “That was tough.”
How quick Goepel got sick caught all of her co-workers off guard. It made the pandemic personal, Kilian said.
Little is known about how the coronavirus affects pregnant women in the U.S. A report by the Centers for Disease Control and Prevention released on June 26 — the day Demi was born — found pregnant women are at a greater risk of severe illness with COVID-19 than women who aren’t pregnant.
As of July 7, over 3,250 pregnant women with COVID-19 have been hospitalized and 31 have died, according to the CDC.
The numbers, however, are likely understated given how pregnancy status is often missing from case reports, researchers warn. The reasons for hospitalizations and deaths are also not known. The CDC says it’s working with local health departments to collect better data to understand COVID-19 and pregnancy.
BJC HealthCare, which includes Barnes-Jewish Hospital where Goepel was a patient, reports having cared for 10 pregnant women hospitalized with complications from COVID-19.
“Knowing Mallory was healthy and young and to see her go through that was very scary,” Kilian said. “To see someone as strong as Mallory get hit that hard was very emotional for all of us.”
No kiss or hug
On Sunday, June 14, Goepel started coughing. She had been outside and swimming in the family’s backyard pool. Maybe it was just allergies, she thought.
By that evening, however, her cough got worse. The next morning, she was supposed to go to work. Instead, she went to a drive-thru COVID-19 testing site at the St. Louis Children’s Hospital Specialty Care Center in west St. Louis County.
By 6 p.m., she found out she had tested positive.
Her husband, Kyle Goepel, said he felt a mix of shock and anger. The couple were young and healthy. They had been social distancing. They had no idea how she became infected.
“I didn’t know anybody, no one, not friends of friends of friends … that had tested positive,” said Kyle, also 35. “And here I am, my 32-weeks pregnant wife tests positive.”
Throughout that day, Mallory’s symptoms grew worse: extreme fatigue, stuffy nose, chest pain, shortness of breath, fever and a horrible cough.
She isolated herself upstairs in her room. The rest of her family were tested two days later. Kyle was positive. The kids tested negative at first. Negative tests, however, can sometimes be wrong. They were tested again a week later, and those came back positive.
“No one was able to come help,” Mallory said. “Everybody wanted to, but we were in quarantine.”
Kyle ended up having mild symptoms, while their children showed no symptoms.
That week, Mallory had roller-coaster days — feeling better at moments, then horrible again. “I never felt so sick in my life,” she said. “It’s way, way worse than the flu.”
On June 20, five days after testing positive, Mallory began to feel better. She thought she was finally over it. Around dinnertime, however, the shortness of breath came back.
And it didn’t go away.
Kyle got the kids to bed. His parents came with gloves and masks and sat in the living room. Around 9:30 p.m., Kyle drove Mallory to the emergency room at Barnes-Jewish Hospital.
He dropped her off and, not thinking, rushed to park the car. He would later play that moment over in his mind and berate himself.
“I’m a very affectionate person. I hug and kiss, that’s what I do,” Kyle said. “I was mad at myself, like, ‘You idiot, you didn’t even think about it. You didn’t give her a kiss or a hug.’”
They forgot he wouldn’t be able to come in the hospital with her.
On the drive home, Kyle was worried, but he believed what he planned to tell his children — that Mommy just needed a little oxygen, that she would be home soon.
Mallory thought the same thing, she said. “I had absolutely no idea what was about to happen.”

Mallory Goepel, pregnant with COVID-19, went to the emergency room on June 20 when she began to struggle to breathe. A chest X-ray revealed she had viral pneumonia, a serious complication of COVID-19. “When I saw that X-ray, I knew I wasn’t going anywhere,” said Goepel, who works as neonatal intensive care nurse. Photo provided my Mallory Goepel
‘You need to fight’
Because of her chest pain, pregnancy and days in bed, doctors feared Mallory was at risk of a pulmonary embolism — a deadly blood clot in the lungs. They decided a CT scan was necessary, despite the radiation exposure.
Thankfully, there was no clot. An X-ray, however, revealed she had severe pneumonia. “When I saw that X-ray, I knew I wasn’t going anywhere,” Mallory said.
Within six hours, her oxygen levels had dropped. She needed oxygen tubes to her nose. She was moved to intensive care.
The following days felt like a fog, Mallory said. The amount of oxygen in her blood continued to drop. She had a painful cough and fever. She slept a lot.
She would video chat with her family when she could, trying to keep the conversation light. Her 2-year-old son, Will, didn’t understand the seriousness. However, her typically well-behaved and happy 4-year-old daughter, Gia, began to act out and struggle with sleep.
Kyle said he watched lots of “Despicable Me” movies with the kids. They colored pictures and picked flowers for mom. He tried to stay positive.
Dr. Jennifer Alexander-Brett knew Mallory was coming up on a critical time. After having taken care of lots of COVID-19 patients, she had learned this was when things could take a turn for the worst.

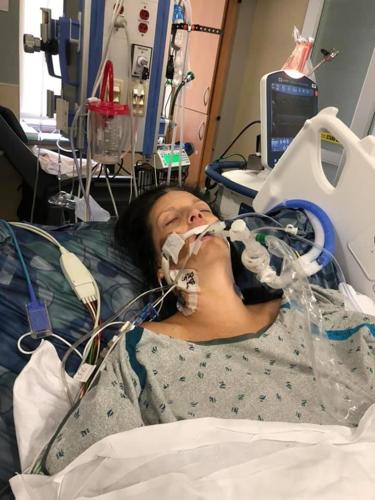
When COVID-19 made it impossible for her to breathe on her own, Mallory Goepel had to be intubated and deliver her baby at 33 weeks gestation via C-section on June 26. Goepel, 35, was on a ventilator for three days after the surgery at Barnes-Jewish Hospital. Photo provided by Mallory Goepel
“There’s a subset that can rapidly deteriorate, and when it happens, it’s very dramatic,” Alexander-Brett said. “We need to act quickly.”
All week, Alexander-Brett had been preparing Mallory and Kyle for this possibility. Because Mallory was pregnant, the doctor couldn’t try typical treatments like: placing her on her stomach to expand the lungs, monitoring her with frequent X-rays or giving her remdesivir, an antiviral shown to reduce severity of COVID-19 but not yet studied during pregnancy.
On June 26, six days after entering the hospital, Mallory’s oxygen level dropped dramatically. The nasal tubes had been providing air that was 40% oxygen (room air is 20%), Alexander-Brett said. The level was increased to 100%, but she could not get enough.
She was over 33 weeks pregnant at that point. A team of doctors decided putting Mallory on a ventilator and delivering the baby was safest for them both.
Mallory panicked. Her parents rushed from Kansas City. Early in the pandemic, nearly 90% of COVID-19 patients who required mechanical ventilation ended up dying, reports said. Some recent research shows that has improved to 36%, still a frightening number.
Kyle and her children couldn’t come to the hospital because they were still infectious. She had to talk to them through FaceTime on a cellphone. She was petrified, crying and struggling to breathe.
“I don’t even remember the conversation to be honest,” Mallory said. “I just remember telling them how much I loved them all.”
Her parents were able to be with her, which was comforting. It was the first time she had seen her dad cry.
Mallory remembers Kyle saying he wished he had given her a hug. “You need to fight now and get back to our family, because you got some kids waiting for you,” he told his Mizzou college sweetheart and wife of 11 years.
“You got to get home to us,” he said, “because I can’t do this on my own, nor do I want to do it with anybody else.”
‘Pure joy’
Demi was born at 3:40 p.m. and weighed 5 pounds, 7 ounces.
“Demi is a fighter just like Mallory,” said Kilian, the nurse manager. “When that girl was born, she screamed louder than I’ve heard a preterm baby scream. It was a great moment to hear that.”

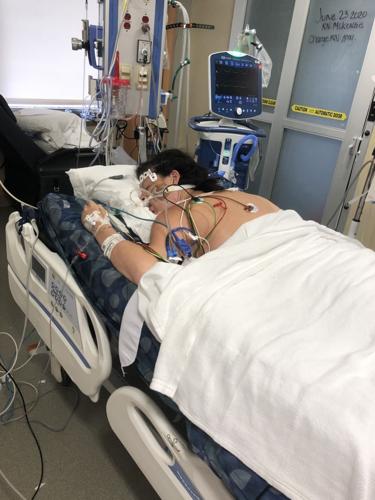
Mallory Goepel, 35, was placed in the prone position after delivering her baby June 26 via C-section and requiring a ventilator to stay alive. The position helps a patient’s lungs expand. Goepel was on a ventilator for three days before recovering. Photo provided by Mallory Goepel
Doctors placed Mallory on her stomach, despite her C-section. She was sedated while the breathing tube did its work. She needed two blood transfusions and multiple medications to prevent blood clots and regulate her blood pressure and sugar. She was able to take remdesivir.
After the first 24 hours, she began to improve.
“She really just couldn’t get over the hump until we did the delivery,” Alexander-Brett said. “Once we did, we were able to aggressively manage (the disease) and get her turned around.”
Mallory was thankful she was far enough along in her pregnancy that Demi fared well. She feels she went into the operating room just as she was about to fall off a cliff. She says Alexander-Brett saved their lives.
Alexander-Brett credits the entire medical team.
Mallory woke up three days later, after her breathing tube was removed.
She immediately wanted to FaceTime with her family. Again, she can’t recall what she said, just an overwhelming sense of relief and happiness.
She could hardly talk from the breathing tube passing though her vocal chords. She could hardly smile, but she did. {span style=”background-color: #deffde;”}
Kyle also remembers being overwhelmed. “That feeling was such an emotional high. It was amazing, pure joy,” he said. “I don’t want to say it was worth going through, but that moment of happiness will remain with me for the rest of my life.”
He and the kids celebrated. He had a few cocktails. They played the “Despicable Me 3” soundtrack, which has classic hits like “Bad” by Michael Jackson and “Take on Me” by A-Ha.
“We danced all over the house that night,” he said. “It was a great night.”

Mallory Goepel holds her baby, Demi Penelope, for the first time in the NICU at St. Louis Children’s Hospital on July 2, six days after delivering her via C-section while intubated for COVID-19. “She looked like a perfect angel,” said Goepel, who was worried she might not ever see Demi. Photo provided by Mallory Goepel
Coming home
Mallory’s incision was extremely painful from having been on her stomach. Coughing after having the breathing tube made it worse. But she powered through her physical therapy, weaned off the oxygen and started eating again. Three days after waking up, she was ready to move out of intensive care.
Mallory was able to convince her doctors to let her go home instead. She had to hold her new baby, see her husband and kids.
Nurses wheeled her down to the lobby, where Kyle was pacing. He felt like it was their first date, he said. Mallory started crying before she even saw him.
He bent down and got the hug he had been wishing for. He thought he was going to lose her, he told her, that his life would be ruined.
“He was just so happy to have me back,” Mallory said.
They immediately drove next door to St. Louis Children’s Hospital to see Demi for their first time. She was 6 days old.
They had seen pictures and video, but nothing compared to cradling her soft skin, hearing her gurgles and laughing together about how she looks just like her big sister.
Mallory didn’t want to leave, but she knew she had two others waiting to see their mom. When she pulled up the driveway and got out of the car, they screamed, “Momma!” and ran to meet her. “They gave me huge hugs, probably too hard of hugs,” she laughed.
Demi has tested negative for the coronavirus, Mallory said.
The spread of the coronavirus from mother to fetus is possible but uncommon, research has found. Little is known how infections impact the fetus at different stages of development, or newborns.
Breastfeeding is considered safe. Mallory is grateful her nurses used a breast pump to stimulate her milk supply while she was on a ventilator so she could breastfeed Demi.
Mallory is still weak and feeling abdominal pain. Since leaving the hospital July 2, she has spent her days at the NICU with Demi waiting for her to gain weight and learn to eat on her own.
Mallory and Kyle said the support from others has been humbling. Friends started delivering meals the day she was diagnosed. People sent toys, snacks and gift cards. Mallory heard from sorority sisters, high school friends she hadn’t seen since graduation and others she didn’t even know.
“I am a 35-year-old mom of two who was pregnant and working in health care, and this happened to me,” she said. “I think it really scared and brought to light the seriousness of this all for a lot of people.”
Weighing 6 pounds and able to eat on her own, Demi got to go home on Thursday. Mallory picked through the preemie outfits friends had sent and settled on a mint green sleeper with “Little Sister” on it.
As Kyle carried Demi into the house in her car seat, Gia and Will clamored to meet their new sister. The siblings sat on the couch so they could hold her.
Mallory placed Demi, sleeping, in Gia’s arms as Will looked on. Mallory couldn’t believe she was seeing them all together. Her nightmare was finally over.
“No cry!” Will said to his mom.
Mallory smiled, “They are tears of happiness, baby.”

Kyle Goepel pushes his wife, Mallory Goepel, and newborn child Demi out of St. Louis Children’s Hospital after the baby was discharged from intensive care on Thursday, July 16, 2020. Goepel gave birth to Demi via C-section on June 26, 2020 when she was on a ventilator being treated for COVID-19. Thursday was the first day baby Demi was brought home and introduced to her siblings. Photo by David Carson, dcarson@post-dispatch.com

Gia Goepel, 4, runs over to get a first look at her newborn sister Demi Goepel as her father, Kyle Goepel, and mom, Mallory Goepel, arrive home on Thursday, July 16, 2020. Goepel gave birth to Demi via C-section on June 26 when Goepel was on a ventilator being treated for COVID-19. Demi was discharged Thursday from the intensive care unit at St. Louis Children’s Hospital and allowed to go home to meet her siblings. Photo by David Carson, dcarson@post-dispatch.com

Family members surround newborn Demi Goepel as she is welcomed home to her family’s house in Des Peres on Thursday, July 16, 2020. Photo by David Carson, dcarson@post-dispatch.com

Mallory Goepel gives her newborn Demi a kiss as Demi’s siblings Gia Goepel, 4, and Will Goepel, 2, meet the baby for the first time at their home in Des Peres on Thursday, July 16, 2020. Goepel gave birth to Demi via C-section on June 26th when Mallory was on a ventilator because she was being treated for COVID-19. Thursday Demi was discharged from the intensive care unit at St. Louis Children’s Hospital and allowed to be brought home to meet her siblings for the first time. Photo by David Carson, dcarson@post-dispatch.com

Mallory Goepel holds back tears as she and her husband Kyle Goepel introduce baby Demi to her siblings Will Goepel, 2, and Gia Goepel, 4, at their home in Des Peres on Thursday, July 16, 2020. Goepel gave birth to Demi via C-section on June 26 when she was on a ventilator being treated for COVID-19. Demi was discharged Thursday from the intensive care unit at St. Louis Children's Hospital and allowed to be brought home to meet her siblings for the first time. Photo by David Carson, dcarson@post-dispatch.com

Newborn Demi Goepel is doted on by her siblings Gia Goepel, 4, and Will Goepel, 2, who is reaching in to put a his baby doll's blanket on his new sister at their home in Des Peres on Thursday, July 16, 2020. Demi was discharged Thursday from the intensive care unit at St. Louis Children’s Hospital and allowed to be brought home to meet her siblings for the first time. Photo by David Carson, dcarson@post-dispatch.com

Mallory Goepel spends a quiet moment with her newborn Demi Goepel at the family's home in Des Peres on Thursday, July 16, 2020. Goepel gave birth to Demi via C-section on June 26th when Goepel was on a ventilator being treated for COVID-19. Thursday Demi was discharged from the intensive care unit at St. Louis Children's Hospital and allowed to be brought home to meet her siblings for the first time. Photo by David Carson, dcarson@post-dispatch.com